You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
As more and more people retain their natural teeth throughout their lifetime, dentists increasingly encounter patients with numerous dental problems associated with tooth wear. Often patients will present looking to improve their smile or with broken restorations, unaware that the underlying cause is functional issues that may also involve tooth wear. If these underlying functional issues are not diagnosed and treated appropriately, any new restorations will also be doomed to fail.
Tooth wear leads to loss of tooth substance. Currently, many dentists are trying to conserve tooth structure rather than use aggressive preparation techniques that lead to further tooth destruction. Modern adhesive techniques, together with new materials, allow the preservation of tooth structure while still producing a restoration that can withstand the forces placed on it. It should be remembered, however, that if the tooth structure is sufficiently challenged, a restoration may need to be provided that protects the remaining tooth structure.1-3
Minimally invasive dentistry involves providing the least amount of dentistry possible while fulfilling the needs and desires of the patient. Sometimes, however, traditional restorations and traditional preparations must be done to protect and conserve remaining tooth structure. Also, some patients may have high esthetic demands and it may be necessary to do more preparation than desired to produce the esthetic result that the patient demands. That would be a balance of risks and benefits that should be discussed very carefully with each patient.1-3
The key to minimally invasive dentistry is to understand that it is always based on a complete examination, diagnosis, and treatment plan for the patient. Once the relevant records have been collected and a diagnosis is made, it is then possible to design where the teeth need to reside in the face of the patient to provide optimal health, function, and esthetics. Once having the design, appropriate procedures and materials can be discussed with the individual patient, dependent on their needs and esthetic requirements.
It is also very important to be clear on the goals for treatment. Often, the aim is to provide restorations that will last for the longest period of time, which in itself is a worthy goal to have. This must be balanced against the possibility of the restoration failing catastrophically, possibly requiring extraction. However, if the goal is to keep the patient looking great with healthy teeth for the rest of their life, restorations should be provided that are less destructive, but may require more repair over the lifetime of the patient. In that case, when the restorations do fail, they may be repaired easily and appropriately.
RESOLVING TOOTH WEAR ISSUES
Often in tooth wear cases, full mouth rehabilitation is suggested or required. With traditional restorations, this can be both invasive and expensive. Using minimal preparation and adhesive restorations can reduce the amount of tooth structure that needs to be prepared, as well as reducing the cost to the patient. The patient needs to understand that, although the initial cost may be reduced, there may be more ongoing costs in repairing these restorations in the future. Both practitioner and patient need to understand the implications of the restorative cycle. With traditional crown preparation, when these restorations fail, a root canal is often required, or perhaps extraction. If the amount of preparation necessary can be minimized, hopefully enough tooth structure can be kept to provide further restorations. This reduces the number of times that a restoration needs to be replaced throughout the lifetime of a patient, giving a better chance of lifetime success. Occasionally, adhesive restorations can be placed as a long-term restoration. Sometimes it can be placed as a temporary restoration, understanding that, in the future, it will need to be replaced by a more traditional restoration. This allows treatment to be phased in over time, which can also be very helpful for patients not only to test the esthetics and function of the treatment being recommended, but also economically.
Over the years, many techniques have been suggested for treating the worn dentition, each often presented as if they are the sole solution. Patients have differing needs and requirements; therefore, having multiple treatments available makes much more sense. One way that has been suggested is to open the vertical dimension providing space for the restorations. That requires at least one full arch of restorations, which can be expensive for the individual. Another method that has been presented is providing a facial restoration to improve esthetics and then to provide a palatal restoration to improve occlusion and function. Although this may be conservative, it can also be expensive; cost-effectiveness must always be considered.
The Dahl principle is another method that has been used successfully over the years to reverse the dentoalveolar compensatory process providing space for restorations. Traditionally, this was a chrome cobalt or stainless steel denture placed on the palatal surface of the teeth. Today, composite restorations are usually placed to perform the same function. Research has shown that using the Dahl principle can successfully create space by addressing localized anterior tooth wear.4 It has been reported that 40% of the space is generated by intrusion of the anterior teeth with 60% of the space created by overeruption of the posterior teeth. It should also be recognized that providing an anterior appliance, such as a Dahl appliance, will act as a deprogrammer and produce space by allowing the muscles to relax and the condyles to seat. The Dahl appliance also improves the torque of the anterior teeth, which improves the overjet, which in turn will help to provide better anterior guidance, particularly an anterior guidance that is in harmony with the envelope of function.4 Direct composite restorations placed using the Dahl principle to treat tooth wear have demonstrated a success rate ranging from 94% to 96% over a 30-month period.2,3
Another method for reversing dentoalveolar compensation and overeruption of worn teeth is to use orthodontics. Orthodontics can move the teeth to a more favorable position, creating space for restoration with a minimal approach by addition.5 Alternatively, gingival margins can be corrected with crown lengthening, then by providing crowns to restore the teeth, which is potentially more invasive.6 The combination of orthodontics and minimally invasive and esthetic restorations can be a very powerful tool in the treatment of tooth wear cases.
Another method to gain space for provision of restorations for the worn dentition is to change the condylar position.7 There is much research that demonstrates that using centric relation will not only provide space for anterior restoration, but will also provide a stable starting point for a reorganized occlusion.8 In turn, this will make restorations more predictable and manage the forces on them in such a way that may increase their longevity.
Long-term success of any of these approaches, regardless of the techniques and materials selected, requires understanding and correction of the underlying problems that contributed to the problems in the first instance. Therefore, to provide patients who present with tooth wear the most affordable, appropriate, longer lasting, and effective treatment as possible, clinicians need to understand the fundamental concepts of occlusion and the forces acting on the teeth. They also need to understand adhesion and restorative design to provide the most appropriate treatment. This involves a complete dentistry approach providing anatomical, functional, biologic, and esthetic results with the teeth, masticatory muscles, joints, and proprioception working in harmony with each other.5,7,9 This will allow the solutions that we provide to achieve the most long-lasting and beautiful results.
UNDERSTANDING COMPLETE DENTISTRY
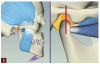
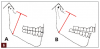
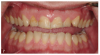
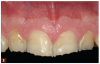
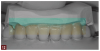
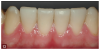
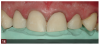
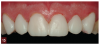
Complete dentistry has very clear goals: function and anatomic harmony, as well as biologic and esthetic success. As teeth wear, the occlusion of the patient will change. When we need to restore the worn dentition, where should we start? As mentioned previously, centric relation is described in much of the literature as the starting point for any reorganized approach (Figure 1 and Figure 2).8 We also must understand how we need to make the new restorations and the existing teeth fit together to make the patient comfortable and provide a functional occlusion. Although variations have been suggested, it is usual to provide equal intensity stops on all the teeth with a cusp fossa relationship. The desire is to create immediate disclusion (Figure 3) and also to establish a guidance that discludes the posterior teeth, but works in harmony with the envelope of function of the patient (Figure 4).4,5 Providing such an occlusion will not only increase the comfort of the patient and the longevity of the restoration, but also decreases the forces acting on the restorations. Although no restoration will last forever, providing such an occlusion will increase restoration longevity, improve patient comfort, and increase both predictability and chances of success.10 This would be true whether the restorations are traditional or more minimal. Whichever way is chosen to proceed, decreasing the forces acting on these restorations is bound to be beneficial (Figure 5 and Figure 6). When choosing between traditional or more minimal adhesive restorations, research has shown that, over a 10-year period, there is little to choose between the two.11,12 It also shows that the failure of more traditional restorations, particular ceramometal restorations, however, is often associated with a more catastrophic, costly, and damaging effect for the patient, whereas using a more minimal approach will often allow restorations to be repaired rather than causing significant issues to the patient.
TREATMENT PLANNING PROTOCOL
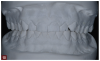
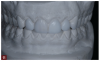
Treating a patient with a worn dentition, as any other condition, uses four steps. We always begin with a thorough examination (Figure 7) and record collection using photographs, models, bite registration, and facebow recording (Figure 8 through Figure 10). This information forms the basis for diagnosing the problems of the patient and allows us to find a stable starting point for our potential solution. The information is also used in our two-dimensional visualization of where the teeth need to reside in the face of the patient to produce optimal function and esthetics, which is the second step. Once the case has been visualized, it can then be converted to three dimensions, using either a traditional diagnostic wax-up (Figure 11) or a virtual wax-up on a computer. Once the design has been decided on, the materials and procedures that are most appropriate can be discussed with the patient. Criteria for the most appropriate treatment approach may be predicated on what existing restorations are present and how much tooth substance remains, and the esthetic requirements as well as the economic situation of the patient.7 Often with worn teeth, the remaining tooth structure is already smaller than the prescribed future tooth shape; therefore the remaining tooth structure can often be increased. This can be described as a solution-driven preparation.
Once we understand where the new tooth needs to reside in space, we often realize that further tooth substance reduction is not necessary. The diagnostic wax-up is used to produce matrices that can be used to make the provisional restorations (Figure 12 through Figure 15), the third step, which in turn drives the position of the final restorations and the position for implant placement or orthodontic movement. Once the provisionals have been approved for esthetics by the patient and the function has been determined by the clinician, then this information can be conveyed to the laboratory so the restorations can be completed. Traditionally, this would be done through photographs, impression of the provisional restorations, bite registration, and facebow registration. Again, now, through the use of digital impressions, there are new and exciting ways of copying the contours and esthetics that we have produced in the provisional restorations. This approach leads to predictable results, as the patient has tried and approved the provisionals before moving to the final restorations, the fourth step (Figure 16 and Figure 17). This makes the whole procedure predictable, efficient, and productive. Considerable evidence in the literature also supports this approach for treatment of the worn dentition.10-13 Muts and colleagues13 described the use of diagnosis waxing and diagnostic tooth arrangements, as well as centric relation for rehabilitation of the worn dentition. They also suggest a provisional stage before the definitive treatment to adjust and improve the design of the definitive restorations, which may be either composite or glass ceramics.
CONCLUSION
When faced with treating patients with worn teeth, it is incumbent upon the dentist to provide the optimal solution for each patient. That will undoubtedly involve more than one way of helping the patient. Although minimally invasive treatment is a very important option today for conserving tooth structure, it should also be remembered that minimal does not mean no intervention. Also, while desiring to do as little as possible, we also need to do as much as we need to meet the requirements of the patient. Obviously, it is extremely important that after treatment planning, the options and the risks and benefits of each option are discussed and understood by the patient. Understanding the complete dentistry process and occlusion is the key to providing minimal cost-effective, predictable, long-lasting, and esthetic restorations that are appropriate for each individual.
REFERENCES
1. Kubo S. Longevity of resin composite restorations. Jpn Dent Sci Rev. 2011;47(1):43-55.
2. Hemmings KW, Darbar UR, Vaughan S. Tooth wear treated with direct composite restorations at an increased vertical dimension: results at 30 months. J Prosthet Dent. 2000;83(3):287-293.
3. Poyser NJ, Briggs PF, Chana HS, et al. The evaluation of direct composite restorations for the worn mandibular anterior dentition – clinical performance and patient satisfaction. J Oral Rehabil. 2007;34(5):361-376.
4. Briggs PF, Bishop K, Djemal S. The clinical evolution of the ‘Dahl Principle.’ Br Dent J. 1997;183(5):171-176.
5. Dawson PE. Centric relation. Its effect on occluso-muscle harmony. Dent Clin North Am. 1979;23(2):169-180.
6. Seixas MR, Costa-Pinto RA, de Araújo TM. Gingival esthetics: an orthodontic and periodontal approach. Dental Press J Othod. 2012;17(5):190-201.
7. Dawson PE. Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2007.
8. Keshvad A, Winstanley RB. An appraisal of the literature on centric relation. Part I. J Oral Rehabil. 2000;27(10):823-833.
9. Dawson PE. New definition for relating occlusion to varying conditions of the temporomandibular joint. J Prosthet Dent. 1995;74(6):619-627.
10. Magne P, Magne M, Belser UC. Adhesive restorations, centric relation, and the Dahl principle: minimally invasive approaches to localized anterior tooth erosion. Eur J Esthet Dent. 2007;2(3):260-273.
11. Smales RJ, Berekally TL. Long-term survival of direct and indirect restorations placed for the treatment of advanced tooth wear. Eur J Prosthodont Restor Dent. 2007;15(1):2-6.
12. Bartlett D, Sundaram G. An up to 3-year randomized clinical study comparing indirect and direct resin composites used to restore worn posterior teeth. Int J Prosthodont. 2006;19(6):613-617.
13. Muts EJ, van Pelt H, Edelhoff D, et al. Tooth wear: a systematic review of treatment options. J Prosthet Dent. 2014;112(4):752-759.
Disclosure
Dr. Buckle is the Director of the Dawson Academy, UK.
About the Author
Ian Buckle, BDS
Private Practice, Wirral, England