You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Every dental team has experienced it. The proper steps are taken in a typical crown-and-bridge appointment: anesthesia administration, careful preparation, and retraction. The tray is selected, the impression material is mixed, the low-viscosity material is injected, and the tray is seated. The appropriate amount of time is allowed for the material to set. However, upon removal and inspection of the final impression, the dental team finds it falls short of clinical expectations. Worse, sometimes the team may think the impression is good, only to receive the dreaded phone call from the dental laboratory, saying that the impression lacks the necessary detail for the laboratory to proceed with the case.
While a myriad of excellent material options today are available, making optimal final impressions still a challenging task. Any laboratory will confirm that technicians are routinely challenged by final impressions that lack either the detail necessary for them to see the marginal areas or the necessary occlusal morphology required to accurately mount the casts. The purpose of this article is to review a specific protocol that will create a predictable path to taking accurate master impressions.
The Goal of an Accurate Master Impression
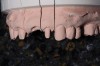
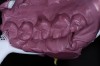
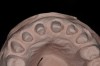
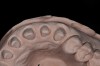
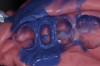
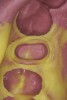
It is important to remember that the purpose of a master impression is to create a master model on which qualified laboratory technicians will fabricate restorations to serve the esthetic, functional, and biologic requirements of the patient. With that in mind, it is critical that upon removal of the impression, it be closely evaluated. The final impression should capture all the surfaces of all the teeth and extend to the mucobuccal fold (Figure 1). If a maxillary impression is made, a good representation of the palate is also important. The occlusal surfaces of all the teeth should be captured in detail (Figure 2). The impression should be free of pulls, voids, and air bubbles (Figure 3). The preparations should be clean, crisp, and free of contamination; in addition, the impression material should have flowed 0.5 mm past the margin circumferentially around the tooth (Figure 4 through Figure 7).
It is important to remember that the more information the laboratory technician has, the better job he or she can do. When working on a case such as a simple lateral incisor, the technician wants to see a clean, crisp, ideal preparation, as well as the entire contour of the opposite side of the dentition. A good ceramist will study both the shape of the tissue and the specific contours of the contralateral tooth. Studying the specific shape of the root at the margin makes it possible to create an emergence profile that will mimic a natural, self-cleansing form, but only if the details have been captured in the impression itself.
Start with Healthy Tissues
Nothing makes the job of the dental team easier than taking the time necessary to create a healthy environment prior to the restorative phase. Inflammation of the gingival tissues is the enemy of the restorative process. Bleeding and contamination from the crevicular fluid will compete for space with the impression material within the sulcus, leading to indistinct preparations and lack of detail at the margin. Further, inflamed tissue is unstable tissue that will likely recede. Simply put, trying to proceed with restorative dentistry in an unhealthy environment is one of the biggest compromises a dental team can make.1 Making sure the root surfaces are free of plaque-related etiologies, that the tissues have had time to respond to initial therapy, and that the patient has been instructed on appropriate home care modalities is critical to the success of this endeavor.2
Patients with old restorations or caries at or below the gingival margin should be closely scrutinized. Often these deficient areas are within the biologic width, making it nearly impossible to impress these areas. Furthermore, even if an accurate impression is captured in this scenario, the long-term health of the patient will be compromised. In these situations, it is wise to eliminate the defective areas, as well as to create an optimal periodontal environment (through periodontal surgery), prior to the restorative phase.3
Lastly, taking time to get the occlusion ideal prior to the restorative phase is also important for tissue stability. Traumatic occlusion schemes can lead to wear, mobility, and migration of the dentition. These signs of instability in the presence of bacteria can lead to the kinds of tissue problems previously described. Following a comprehensive approach to provide occlusal stability, as well as optimal periodontal health prior to the restorative process, is critical for predictable long-term success.
Create an Impressible Preparation
While the nuances of tooth preparation go beyond the scope of this article, the better the tooth is prepared, the better the final restoration will be upon completion. Laboratories struggle—even with perfect impressions—when the prepared teeth are rough, irregular, and lack a consistent marginal design (Figure 8 through Figure 13). It is important to take the time to properly build teeth up; create an optimal amount of buccal, interproximal, lingual, and occlusal reduction; and provide a clean, crisp margin. Dental team members who are consistent in this process will quickly learn to read their own impressions to see if they have met the aforementioned requirements. In addition, the laboratory technicians upon whom dental teams rely so heavily will also be able to predictably determine if the master impression/cast is clinically acceptable to enable them to proceed.
Retract with Intention
If care has been taken to get the mouth healthy, tissue retraction should not be difficult. The goal is to provide circumferential access to the root surface of the prepared tooth 0.5 mm apical to the definitive margin. This requires mechanical displacement of tissue in a manner that will not cause bleeding or seeping of the crevicular fluid. The following options are used in restorative dentistry.
Retraction Cords
These have been used in dentistry to mechanically displace the periodontal tissues for decades. Many have used the two-cord technique with great success. The cords can be used plain or soaked in hemostatic agent. The first, smaller cord is placed carefully into the base of the sulcus to eliminate the seeping of crevicular fluids. A second, larger cord is placed on top of the first, with the purpose of mechanically displacing the sulcular tissues. Five to 10 minutes is required for retraction to be accomplished; after that, the top cord is removed, and the impression can be made.1,4
Electrosurgery
This technique has also been used to create a trough around the tooth into which impression material can be flowed. While this modality allows for efficient removal of the soft tissue, care must be taken to not cause irreversible harm. The tips of a standard electrosurgery unit cut at the tip as well as the sides. This design can create a broad zone of necrosis, and can contribute to the loss of tissue height in thinner periotypes.5
Microlaser Retraction
Various laser wavelengths are used for the purpose of retraction, but most common among them is the diode. The benefit of the laser is that the energy levels can be set to remove very small amounts of tissue at a time. This, in combination with the fact that the laser will only cut on the tip and not on the sides, allows for a great deal of control. The author has found that the use of laser energy—in conjunction with high magnification through a dental microscope—allows the creation of an ideal and conservative trough in which impression material can flow.
Chemical/Mechanical Options
There are several materials that provide a displacing agent (clay or putty) combined with hemostatic agents to inject into the sulcus. These materials are best used as an adjunct to the previous techniques.
Tray Selection
While some dental teams routinely use custom trays, many successfully use stock trays. The key is to fit the tray to ensure that there is a minimum of 2 mm to 3 mm between the tray and the areas to be impressed. All trays should be rigid and have the capacity to support the impression material.6 In addition, if an adhesive is required, it should be carefully painted onto the tray and be completely dry prior to mixing the impression material.7 Unstable impression materials lead to inaccurate dies.
Material Choices
The two most frequently chosen impression materials are vinyl polysiloxanes (VPS) and polyethers. While both can be used with success, dental teams should be aware of the advantages and disadvantages of each material.
Polyethers
Polyether impression materials have been highly successful because of their physical properties, which include hydrophilicity, lower polymerization shrinkage, long-term dimensional stability, highly accurate surface detail, minimal distortion on removal, and adequate tear strength. There are several polyether impression material products from various manufacturers.
However, some of the disadvantages of this category include rigidity (hard to get out of the mouth and difficulty with cast separation) and expense. It is also important to remember that these materials will absorb water if left immersed in disinfectants for long periods, which could lead to dimensional instability.
Vinyl Polysiloxane
Addition-reaction silicones, also known as vinyl polysiloxanes, are the most popular final impression materials in dentistry. These materials exhibit superior tear resistance, neutral taste, variable working and set times, and less rigidity than polyethers (enabling ease of removal from the mouth and cast separation). This last characteristic is particularly important, as removing an impression from the mouth can pose a strong risk of distortion and tearing.
VPS impression materials are better able to handle the stretching and compressive forces that impressions are subject to during this step, with evidence showing them to exhibit better elastic recovery than other elastomers, as well as less permanent deformation (Figure 14).8 These materials also exhibit less polymerization shrinkage (the least of any elastomeric material) and increased dimensional stability. This dimensional stability is due to the fact that the materials are not affected by changes in humidity, and they do not produce any byproducts or undergo further chemical reactions after setting.8 This characteristic makes a VPS impression dimensionally stable for up to 7 days.9 Vinyl polysiloxanes are also easily disinfected in any solution without loss of accuracy.8
The disadvantage of this type of material is that it is less hydrophilic than polyethers and latex contamination can be an issue. As with any type of material, performance can vary by formulation, so dental teams should consider the available data on any product’s toughness and resistance to distortion.
Material Characteristics
Dental teams should consider some additional physical properties that, when understood, can increase the success of this process. This knowledge will also assist in aligning physical properties with the specific clinical challenge that presents.
Viscosity
Viscosity describes the flow characteristics of an unset impression material. Materials with low viscosity have high flow, and those with high viscosity have low flow. Low-viscosity material can be referred to as light-body, syringe, or wash material. These materials tend to flow easily and record fine details. Using a low-viscosity material alone is not indicated as it will run down the patient’s throat and not have enough support to stay in the areas where it is desired. By contrast, a highly viscous material will be extremely stable, but will not have the capability to flow and capture intricate details. While the viscosity preference may vary depending on the dental team’s preference, it is the author’s choice to use as low a viscosity material as possible to syringe, then to support this with material with a high-viscosity tray material to hydraulically push it into the anatomically critical areas. Medium-viscosity materials are ideal for impressions for removable prosthodontics, as they will not run like a low-viscosity product, but will still have enough body to give the clinician the ability to border-mold the peripheral areas as the material sets.
Rigidity
While the rigidity of a polyether can be an issue, there are times it is desirable. Open-tray implant prosthodontic impressions provide an example. When taking a fixture-level impression of multiple implants, any play of the implant impression coping (and implant analog) will lead to inaccuracy. Polyether is an excellent material choice for this restorative challenge. By contrast, if a crown-and-bridge impression is to be made with older bridgework in place, or there are undercuts from buccal exostoses, a polyether is at risk of becoming stuck in the patient’s mouth; a polyvinyl may be indicated in such situations.
Setting Time
The setting time for an impression material is the total time from when the assistant begins mixing the material to when it is completely set and may be removed from the mouth. The working time is measured from the start of the mix until the impression material can no longer be manipulated without distortion. There is a trend in dentistry to move toward faster and faster set times. Generally, the working time corresponds to the setting time. While set times range from 2 to 6 minutes (fast and regular set), a fast-setting material will have a short working time, and a slow-setting material will have a long working time. The key is to align the working time required with the task at hand. If the clinical team is making a master impression for a single crown, faster-setting materials are certainly possible. When the procedure is 6 to 14 units on a crown and bridge or involves a patient who is particularly challenging, maximizing the working time is prudent. Therefore, while shortening the working time may seem desirable, the dental team runs the risk of compromising the accuracy of the master model. Always align the working time of the material with each clinical reality.
A Note on Digital Impressions
There is no question that dentistry has moved into the digital age. Many dental teams have purchased intraoral scanners, which allow them to create chairside CAD/CAM restorations, as well as use a variety of modalities to better create beautifully fitting laboratory-fabricated restorations. It is important to understand that regardless of the method used to create the master model, the criteria for success remain the same. Careful manipulation of healthy soft tissues is a requirement prior to the intraoral scan. Having the ability to carefully check the virtual master model at high magnification on a high-resolution monitor enables the dental team to verify accuracy on the spot (Figure 15). While these and other benefits of digital impressioning exist, it is still unclear when this technology will completely penetrate the market.
Conclusion
Crown-and-bridge procedures are daily occurrences within most restorative practices. The success of these procedures hinges on the precise preparation of the teeth involved, along with the capturing of these details to accurately create the master cast. This article has discussed some specific criteria to consider in order to improve the predictability of creating optimum master impressions.
Acknowledgment
The author would like to thank Bayview Dental Laboratory for providing the photographs for this article.
Disclosure
The author has received material support from 3M ESPE.
References
1. Christensen GJ. Laboratories want better impressions. J Am Dent Assoc. 2007;138(4):527-529.
2. Caffesse RG, Guinard EA. Treatment of localized gingival recession. Part IV. Results after three years. J Periodontol. 1960;51(3):167-170.
3. Hess L. The biologic and restorative interface: improving periodontal health with contemporary materials and sound restorative dentistry. Contemporary Esthetics and Restorative Practice. 2005;9(3):46-51.
4. Cloyd S, Puri S. Using the double-cord packing technique of tissue retraction for making crown impressions. Dent Today. 1999;18(1):54-59.
5. Radz GM. The key to perfect impressions. Compend Contin Educ Dent. 2010;31(6):463-465.
6. Hoyos A, Soderholm KJ. Influence of tray rigidity and impression technique on accuracy of polyvinyl siloxane impressions. Int J Prosthodont. 2011;24(1):49-54.
7. Cho GC, Donovan TE, Chee WW, White SN. Tensile bond strength of polyvinyl siloxane impressions bonded to a custom tray as a function of drying time: part I. J Prosthet Dent. 1995;73(5):419-423.
8. Mandikos MN. Polyvinyl siloxane impression materials: an update on clinical use. Aust Dent J. 1998;43(6):428-434.
9. American Dental Association. Vinyl polysiloxane impression materials: a status report. Council on Dental Materials, Instruments, and Equipment. J Am Dent Assoc. 1990;120(5):595-600.
About the Author
John C. Cranham, DDS
Private Practice
Chesapeake, Virginia
Clinical Director
The Dawson Academy